Snake Bites
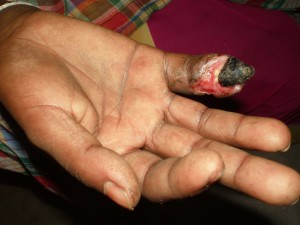
Effects of snake bite on finger
Snake bites are common in most rural areas, particularly in forest and forest fringe villages. Deaths due to poisonous snake bites are a major cause of death in our area despite being highly preventable. Based on an epidemiological survey of 26 villages with a total population of nearly 19,000 individuals in Burdwan district of West Bengal state in India, Hati et al worked out an annual incidence of 0.16% and mortality rate of 0.016% per year . Maharashtra, one of the states of India with the highest incidence, reported 70 bites per 100,000 population and mortality of 2.4 per 100,000 per year. In our area, the annualized snake bite rate is the same as Burdwan at 1.58 per 1000 population, and the annual mortality of 1.3 per 10000 population. The most common snake bite is from the krait, consisting of over 80% of venomous bites in this region. Snake bites continue to kill.
Humans are not the only ones in danger of snake bites. The loss of livestock is a frequent issue in Bilaspur district. Of 25 snake bites in large animals, as many as 12 died. This is a huge problem, as livestock is a major source of livelihood and income for many people living in the region, and such animals are extremely costly to replace.
Despite the high prevalence, awareness around the issue of snake bites remains extremely low. A video clip of a patient with envenomation following a krait bite was shown to the health workers (the patient was seen in our clinic at Ganiyari). Only two of the 104 workers (who had relatives who had died of a snake bite), recognized what it was. Even among the nearly two hundred health workers (doctors, ANMs, and others) who were shown the video clip, only a handful could recognise the symptoms.
It is essential for communities to be able to recognise envenomation early in order to be able to seek help at an early stage. It is also vital that health workers are trained in the management of symptoms. In order to raise awareness about the early signs of snake bite, we also put together a CD with a powerpoint presentation in hindi about snake bites, which has been distributed in the programme villages. We also developed a training in which health workers are made aware of the commonality of the problem and are taught the proper protocols to manage snake bites. Most people kill the snake as soon as it bites someone, and treatment options are limited to “jhaad phoonk” and consumption of herbal remedies. Often the patient is taken to hospital too late to be saved.
In order to spread awareness beyond health workers, JSS conducted a programme on snake bites that was broadcast on the local radio. The programme consisted of a question and answer session, in both Hindi and Chhatitsgarhi. It was broadcast several times over a period of two weeks, and was widely heard in the surrounding villages. Subsequently, patients attending the outreach clinics as well as the clinic at Ganiyari were interviewed about whether or not they had heard the programme, and asked some basic questions about snake bites. 20% of the respondents had listened to the programme. Information obtained during the interviews is being compiled and analysed.
Animal Bites
We maintain that animal bites resulting in death and disability to human and their animals is an overwhelmingly rural problem and these people suffer from gross negligence of our primary health care system. There is a dearth of drugs, vaccine and antisera, as well as information and skill base to manage these at the peripheral outposts. Information regarding the incidence of snake bites among the local communities is also lacking.
In order to address this scarcity of data, we have been documenting the prevalence of animal bites since August 2008 in 54 programme villages, consisting of a total population of 26565. Information has been collected from all sources- the health workers who come for their monthly training programmes, the senior health workers when they visit the individual villages on their beat programme, and the field coordinators who hold nukkad or hamlet level meetings. While house to house surveys have not been done, we feel that the current data for snake and suspected rabid animal bites accurately reflects the incidence in the community. Data on scorpion and bee/wasp bites has not been officially collected due to the incredibly high frequency and low reporting of such incidences.
The average yearly incidence of dog and cat bite/scratches in an Italian clinic was 58.4 and 17.9 cases per 100 000 residents, respectively. In a clinic in Pittsurgh, Pennsylvania, the bite rate was 12.9 per 10000 persons (95% confidence interval [CI], 10.5-15.4). According to data collected over a period of 10 months, the rates in Bilaspur, India are more than four times higher, with a yearly incidence of 51.9 per 10000 population.
The WHO has sponsored a national multi-centric rabies survey to find out the incidence of animal bites and anti-rabies treatment practices. Twenty-one medical colleges chosen with geoscatter representation conducted the survey during February-August, 2003. The survey was conducted in 18 states, covering a population of 52,731 chosen randomly from 8500 households. The annual incidence of animal bites was as high as 18 per 1000 population in rural areas, which is certainly much higher than our area. The same group also concluded that the annual incidence of rabies is 2 per 100000 population. This year we have already lost one person due to rabies and at least 25 livestock in 10 months, which has caused a significant burden to the families involved.
What does not seem being of obvious importance, we saw a large amount of livestock and other draught animals’ mortality due to these suspected rabid animal bites. In this same population’s livestock, we saw them losing 25 animals in these 10 months, which causes significant economic burden on the people.
Scorpion and Other Bites
While our data on scorpion and bee and wasp bites is not complete, we did have one death among 43 scorpion stings among humans (1.93 per 1000 population). One cow also died from a scorpion sting during this period. This should be factored in for considering the importance of animal bites and for resource allocation in the primary health care system.
Similarly, bee and wasp bites were 61 among the people giving an annualized rate of 2.75 per 1000 population.
Improving Treatment

Animal bite training
Taking cognizance of the problem of animal bites, we decided to start animal bite centres at all our sub centres. Here we provide information regarding each animal bite, offer definitive first treatment for its care, and document its burden and pattern carefully.
These animal bite care centres were opened in the months of June and July 2009. There has been a sharp increase in the number of people seeking primary care for the animal bites in all the sub centres in the first 6 months!
We have also been able to design a solar powered refrigerator that has been commissioned at the Bamhni sub centre to be able to preserve the antisera and the vaccines for snake and suspected rabid animal bites. This is has rarely been done in primary health care. The refrigerator has been made at a cost of only Rs 40,000, whereas the cheapest in the market is not available for less than Rs. 125,000. The refrigerator has a volume of 80 litres and has passed the acid test of surviving through the entire monsoon of 2009, where we monitored the inside temperature, which never went over 6 degrees Celsius. The availability of the refrigerator in areas where there is no power or assured regular and reliable voltage power opens solutions for problems like keeping heat labile but life saving drugs like insulin and important reagents like rapid diagnostic kits safe.

