Tuberculosis is the most common killer of young people in rural Bilaspur. It is unfortunately not unusual to see many people in a family affected by the disease due to close contact and a shared status of malnutrition. A recent survey of the scientific literature as well as our own experience have shown us the devastating role hunger can play in tuberculosis. Undernutrition is a frequent cause of immunological suppression, far more than HIV-AIDS and diabetes. The fact that undernutrition is both highly preventable and highly treatable makes the presence of such high rates of tuberculosis and malnutrition not only a common clinical problem, but a major social injustice.
As a group, 90% of our patients are undernourished, and 60% do not have enough food at home year round. Eighty percent of our adult women patients weigh < 40 kg and 20% of them weigh < 30 kg. Ninety percent of our adult male patients weigh < 50 kg and 40% of them weigh < 40 kg. Forty percent are in debt, often due to the cost of treatment, sometimes to the tune of tens of thousands of rupees. Poverty interacts with tuberculosis in a vicious cycle: it makes you more likely to come down with tuberculosis and then it makes it that much more difficult to seek treatment and continue that to completion. Due to decreased host resistance consequent to malnutrition, the poor often have more extensive disease. Moreover, they tolerate anti-tubercular drugs poorly and are more likely to die despite treatment.
Issues in Treatment
We have been arguing for changes to the management of tuberculosis for several years. From our review of the literature and our own experience, we had found intermittent treatment regimens inferior to daily treatment regimens. Fortunately, the World Health organisation now accepts and recommends daily frequency of drug treatment for all types of tuberculosis. The government of India has recently accepted the idea to change the treatment regimens to daily, but it seems it will take at least 2 more years to operationalize this change.
We have also recognized the need for supplemental food in the treatment of tuberculosis. We have been able to make the state of Chhattisgarh to announce a committed budget early in 2015 to ensure supplemental food rations for all patients diagnosed to have tuberculosis. Even at a national level, it is likely that the Central Tuberculosis Division may decide to add supplemental food rations to all tuberculosis patients.
Further Changes Are Needed
We feel that sputum microscopy is a robust, simple and reliable tool that can be utilized for the diagnosis of tuberculosis of the lungs. By examining multiple sputum samples, we diagnose 60% of our patients with tuberculosis of the lungs without an X-ray. The value of sputum microscopy can be significantly enhanced by using simple concentration tools such as the Ammonium sulphate-Sodium hydroxide technique.
We also feel that all newly diagnosed patients should be offered sputum culture so that their drug resistance status be found out . This will allow us to pick up not only multi drug resistant tuberculosis , but also INH resistant disease , which also deserves tailored treatment different from those who have drug sensitive disease. At Ganiyari, we are doing cultures on sputum and other body fluids on all patients that we diagnose. These microbiology investigations are being done with the help of National institute of research in tribal health , Jabalpur and Intermediate Reference laboratory for tuberculosis , Raipur.
To avoid treatment failure or relapse among TB patients, one needs to give more prolonged treatment with daily rather than intermittent regimens. We need to study this in greater detail.
We feel that the socio-economic predicament of the patient needs to be looked into more closely to find out objective predictors of defaulting behaviour. Patients at high risk of default must be counseled more thoroughly than others and also followed-up more assiduously.
Close monitoring of high risk patients has helped us to reduce if not eliminate defaults altogether. In anti-tuberculosis drugs, there is a desperate need for standard formulations, bio-availability related information, assurance of quality, and price control.
Preliminary results from nearly 60 isolated patients suggest that even initial resistance individually to streptomycin, ethambutol and the fluoroquinolones is more than 10%. Acquired resistance levels are far higher.
We need to educate doctors about standard treatment guidelines for tuberculosis. Few formally qualified doctors (MBBS or MD) in Bilaspur prescribe anti-tuberculosis drugs in the right dose or use the correct combination for the appropriate duration.
Case Studies
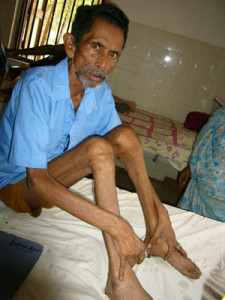
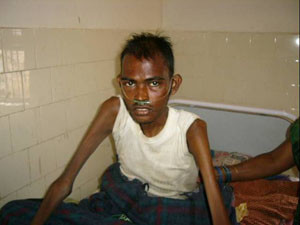
A Family with TB
The gentleman to the left of the picture was the first person in his family to fall prey to tuberculosis. He completed treatment successfully, thanks to a generous grant from the Sir Ratan Tata Trust that allowed us to take a comprehensive look at the social and medical factors that lead poor rural patients with tuberculosis to stop treatment prematurely despite free medicines being made available at government clinics. Unfortunately, after he recovered, his father and sister came down with the disease. Their skeletal features tell us clearly why tuberculosis was once known as ‘consumption’ or ‘kshaya roga’. Fortunately, his father and sister were diagnosed in time and they too went on to make a full recovery.
A Migrant Worker
A patient diagnosed with pulmonary tuberculosis working at a construction site near Aundh in Pune developed symptoms of pulmonary tuberculosis and was diagnosed with the disease at a public health facility in Aundh. She was due to be started on treatment there, but ended up returning to her mother’s house, which was about 75 km from Ganiyari. She came to us for the sake of treatment. She refused numerous offers of referral to the RNTCP in Chhattisgarh, or to the Doctors in Aundh; she said she had faith in JSS because her sister who had previously fallen very ill to tuberculosis had been treated here successfully. She kept up her appointments regularly and only after she completed her 6 months of therapy did she leave again for Pune.
This case illustrates the predicament of migrant workers who develop serious medical problems but are unable to negotiate the processes of seeking care at the local public health facility. Many choose to seek care back home because of the ease of communication in one’s own language and faith in their familiar health care providers.